Starting/declining hormone therapy Nov, Dec, Jan 2018
Hi, this is for people who had active bc treatment in the fall and winter of 2018/19 to discuss further hormone treatment and to support one another in this journey regardless of treatment choices. This is also for ANYONE who would like to participate in a friendly, supportive manner. This is also the place to get as silly as you're capable of. Let it all out here!
I'll start. Most of my info is in my signature, but to recap, dx September 18, lumpectomy October 18, started Anastrazole right after lumpectomy, radiation November/December 18. Since I have started anastrozole, I have experienced a great deal of peripheral neuropathy in my fingertips. I was on chemotherapy three years ago and had neuropathy from that treatment, however it had abated. I am now taking gabapentin for that side effect. I also have really horrible hot flashes, and increasing joint pain. The problem with starting anastrozole before I started radiation is that I don't know if the horrible hot flashes are super horrible because of radiation or because of the drug. I wanted to start soon because both my estrogen and progesterone were in the highest category. When I go to my oncologist next week I'm going to ask to maybe switch medications to see if that helps.
Comments
-
Signing on and marking as a favorite. Thanks for starting this thread!
My info is in my signature too. As of this moment I am halfway through radiation, waiting to start tamoxifen until that's all done and I'm a bit recovered. My goal was to improve my diet and exercise habits before starting the pills, although that's been hard with all the holiday food around and the dark, cold, slippery conditions outside. But I can still drink plenty of water, aim for five servings of fruits and vegetables per day, and climb the stairs in my house a few times in a row periodically throughout the day.I am most worried about blood clots, and felt somewhat reassured to read somewhere recently that the chances are about the same as they are with birth-control pills, which most people seem to take without worrying too much.
0 -
Hi purple cat! I started my hormone tx early, I don't know if that was a good idea or not.
0 -
Thanks, Wised!
Looking forward to good discussions about the next stage in our treatment.
I'll be on AI beginning in mid January. Not sure which one.
0 -
I have my bottle of Tamoxifen ready to start the day after Christmas. I'm adding a statin drug for cholesterol this week; mine is somewhat elevated and I'm a little diabetic, controlled with one metformin a day, so the statin usually is given with that. I also need a blood pressure drug - again, mine is just a little high, but my PCP prescribes it for diabetics. Tamoxifen can raise blood pressure a bit, so it's good to counteract it. Unfortunately, the Lisinopril the PCP ordered is not to be taken by anyone with kidney issues, and I just had one removed in September! So, after asking both my oncologist and the pharmacist about it, I need to get her to change to a different pill. And then I need to shop for a new PCP. So, it will be fun to try to sort out any side effects with three new prescriptions, and adding OTC biotin and chondroitin at the same time!
0 -
Signing in! Will start Femara the second week of January. I hate take any meds and am really dreading this one. Not sure about all the side effects you read about here, sounds pretty awful but maybe I will get lucky and it will be tolerable.....
0 -
In! Marked as favorite. Thank you Wised and so happy that many of us who went through rads together will support one another through this too.
I’m due to start tamoxifen in Jan. because the doc is allowing my husband and I one more “get eggs” cycle.
Will post more later. Requisite Domino pic below! But something new for the new thread here she is posing with my most adorable niece. And the feisty bear we gave her
 0
0 -
Hi, I recently completed chemo. Surgery will be in January. Took first shot of lupron yesterday and starting Femara today. Scared of surgery as well as the harmonal treatment. But keeping faith and trust in positive outcome.
0 -
Egregious, ghostie, Alice, pebbles, so glad you could make it!

Domino,


Being positive, hi and I'm glad you're here to share your experience with femara. If my experience with Anastrazole continues in this direction, that might be one I try. I understand your fear! However, I think that the chemotherapy regimen you just went through is going much harder than femara. Have you met with your surgeon?
0 -
Signing in and saying hello! <waves>

My info is in my signature as well.
As to what the future holds, for now, I'm declining Tamoxifen or surgical/medical suppression due to my Spoonie Life. Instead I'll be doing my best to lose weight, exercise, eat right, and taking DIM as an alternative hormone treatment.
If anyone is curious about my path in deciding on to or not to do Tamoxifen, you can find it here:
"Any Early 40s Declining Tamoxifen?" https://community.breastcancer.org/forum/78/topics/868242?page=1
Thanks for starting this thread Wised! Looking forward to great convos and info in the months to come.
Oh, and who has the Jello-shots???!!!
 They are a must! LOL.0
They are a must! LOL.0 -
Hey all! I am in! I will finish rads mid January- not soon enough!!! And according to my MO I am to start tamoxifen “after radiation” I am not too excited about it but the MO said it cuts my rate of recurrence by 50%. I just really hope my lady bits don’t turn into a painful dry wasteland.
0 -
Hi everyone! I’m in too. I received my bottle of Anastrozole (Accord generic). the day I finished rads, but my MO changed his mind and now wants me to start after the holidays. I’m dreading it! I had been on HRT for about 18 years prior to my diagnosis, and am not looking forward to having my estrogen suppressed further.
Thanks Wised, for starting the thread. It’s great to go through this with others that were close to the same treatment schedule. I’m especially worried about bone health and joint pain, since I already have the start of osteoarthritis. I just started taking Stronitium Support II capsules to try and hedge that problem
0 -
Hello all,
Thank you, Wised, for creating this thread. So many questions and concerns as we all go forward...
I will finish radiation on December 31. I guess it's a good way to end the year, but I think AI will be much worse that radiation. Since I refused chemo my MO said I absolutely must take AI and I think she used a 40% number to cut recurrence. (I am ER +/PR- and maybe that factors in. I have never even asked about that.) Chemo was only going to help by about 5% (and I am 68) so that's why I said no. I have a dexa scan on February 6 and will start the AI after that. I have an appointment this week with a mental health counselor who will change my Zoloft rx to something that will be compatible with whatever they decide to give me. My fingers are already riddled with arthritis and my shoulder is a mess and I am worried that I will lose the ability to do things I enjoy (card making, embroidery, a little sewing, gardening...) I do tend to worry about things before they happen so I am going to have to work harder to not do that. Like Ghostie, I hate taking anything and Zoloft is my only medicine. Now I anticipate I will have to supplement the AI with a boatload of other pills just to help me get through it. Spoonie, thanks for sharing the link to your thoughts.
Take Care, everyone.
0 -
Appyfan, Zoloft IS compatible with AI'S, just not Tamoxifen. I have been on Zoloft for years and continue to take it with anastrozole. If it wasn't for Zoloft I would change to tamoxifen in a heartbeat.
0 -
Hi All
I was diagnosed around last year at this time. First DCIS and a lumpectomy, but the pathology came back to show there were more spots and it had become invasive. So i had bi-lateral mastectomy and decided against reconstruction. Didn't want the extra surgery and I'm quite comfortable with my body. I started Anastrozole in April so have been on it just about 8 months. I'm 62 and have been an athlete all my life, so I was/am most concerned with joint pain as a potential side effect. I've had 5 knee surgeries and have alot of osteoarthritis, but it's very rarely painful. Thus far I've been very fortunate -- I have not noticed any side effects. I know they can start any time and not a day goes by without that thought crossing my mind. I'm concerned about bone loss; will have a dexa in March to see if there are any issues. If so, that could also be a game changer for me. I don't want to take the typically-prescribed bone building drugs as they have some serious side effects. My primary care provider is an integrative medicine practitioner and she would not prescribe them. There is a drug called Fosteum (sp?) and it's a food grade bone building medication, by prescription only, that she is positive about - not sure if anyone else has heard of that or takes it? Anyway, trying not to get ahead of myself and worry about something that may or may not happen. So glad to have the opportunity to hear of others' experiences and share our stories.
0 -
I am going to have surgery in January, probably a double quadrantectomy—I am wondering if anyone can advise me on what happens to your sex life with AIs? The comments I see on various forums are so discouraging but maybe ladies with happy sex lives just don't post—any insights, anyone
0 -
Hi MDRR,
I was really excited about the Fosteum Plus, it seemed to be the answer to help with maintaining your bones. I took Fosteum for a year but had to stop because of stomach pains. I heard that is not a common response to the medication but my pains went away after stopping it. My Dexa Scan showed no improvement after being on it for a year, in fact I had some bone loss.
0 -
Good to hear your experience. If I find I have bone loss issues with my dexa, I'd probably be more likely to be open to trying that since it's food grade, but like with all of this stuff, each of our bodies reacts differently. That's a bummer it wasn't right for you; are you trying anything else?
0 -
Wised and librarygirl - we have a family friend who is in her 50s or 60s, post-menopausal,and was started on an AI and didn't tolerate it well at all and switched to tamoxifen and now she's doing great, no side effects. Any thoughts to switching to tamoxifen?
Purplecat - we have very similar goals in that we're both integrating the diet and exercise with this too. On the plus side, I also heard and my onc confirmed that a good way to avoid blood clots is to exercise / keep moving.
Wised (again) - interesting that my onc said it was fine to start tamoxifen with radiation, and then the radiologist said he didn't want me to and would talk to the onc. It wasn't because they can't be done together, he just said he didn't want me to blame any SEs from tamoxifen on the radiation, better to separate them and deal with one thing at a time! Funny how different doctors differ in their plan and POV.
Egregious - I'm starting similar time to you in mid-Jan. Interestingly for the IVF stims they had me take Letrazole during that time and I tolerated it well but I think it was super low dose and only for 5-10 days.
Alice / ghostie / spoonie / Dani / appyfan / purplecat / librarygirl / egregious / wised good to see you here!
Mdrr / thecargirl / ana001 / beingpositive - please to “meet you". I'm the one who usually accompanies a post with a pic of Domino as she was coming with me to radiation, such started a trend.
Ana001 - this article was encouraging to me: https://www.coveyclub.com/sexuality-breast-cancer/ - I have not started any hormone therapy yet so don't know if that changes when I do, but my husband and I have kept up a happy sex life, even when I was in the midst of radiation treatment. Less frequent obvs. around times I had to heal, and possibly more tender and sweet now than crazy. Sorry everyone if that's TMI, but I am going to try and have that not change with tamoxifen, work around the side effects if we have to. Have to keep a sense of normalcy!
And now to get minds off that, here's Domino expressing how I feel right now about starting hormone therapy. I will do it (I did consider not doing it at all like Spoonie and decided for me I'll give it a go, and also 100% understand why and support Spoonie's decision not to). I will do it, as I think for me the benefits outweigh the risks - had 2 positive nodes and an oncotype of 21 that posted the exact same result with tamoxifen alone vs tamoxifen plus chemo - so since tamoxifen is my ticket out of chemo I feel like I have to give it a go, and hope I can minimize SEs through health/nutrition/exercise as well as I did with rads, but I kind of feel like this about it:
 0
0 -
Hi All! I'm a little ahead of you sisters but I think my experience might offer a valuable perspective. I was 55 and diagnosed with BC (details in signature) January 11, 2018. Surgery March, Tamoxifen April, rads 22 rounds May/June. Tamoxifen made me very emotional and I felt like I was getting sicker--vomiting, no appetite, no energy. August 9th my liver packed in. I now have stage 4 cirrhosis induced by Tamoxifen which is a known hepatotoxic substance. Turns out I had fatty liver (grade 2 so not really serious but certainly something we should have been aware of as I was 6ft tall and 260lbs. At the very least, given my size my liver enzymes should have been checked.) I now need a transplant and am not eligible for a 'cadaver' liver due to my history of BC so can only have a live liver donation and thankfully both of my adult sons are a match. Anyway, back to TX. Before starting it and certainly while taking it, get your liver enzymes checked to see how your liver is coping. I am not a drinker nor do I take drugs of any kind so mine was down to TX. 2.9% of people who take TX get some degree of liver damage. I'm one of those unlucky ones but mine is to the extreme of damage. Anyway, I still need to take an AI as it will reduce my chance of recurrence to about 2% so I am on Letrozole. I am taking the 'hepatic impaired' dose which is 1 every other day and am tolerating it well with no side effects except for the odd 'warm flush' but certainly nothing like menopause tropical moments. In January we will try me on the full dose and monitor my liver which is only functioning at approx. 15%. The transplant team feel my liver may last 2 years but I have to be cancer free for 5 years to have a live liver transplant ( know--the math doesn't work out right?).......they said if it failed sooner they would reassess my case. Anyway friends, Tamoxifen is not liver friendly and while most women tolerate it, although many are left with fatty liver as a result of taking TX, some are made seriously ill and left with life threatening complications. I should add that Letrozole is not associated with liver damage or cirrhosis like Tamoxifen. If I have helped one person out there avoid my experience on TX then my journey has served a good purpose.
0 -
thanks wised for starting the thread!
I'm at the pharmacy waiting to collect my tamox prescription. My onco says I can start either before or during or after rads, that it didnt make a difference but suggested starting on a date that's easy to remember.
Rads start on Thursday so now I'm torn should I go ahead and start or wait till rads are done?
0 -
I finished rads October 4th and didn't start Anastrozole until mid-November. Based on several women's posts I asked my MO if I could start out every other day and she was fine with that. I started it every day December 1st. It really hasn't been too bad. I feel a little stiffer when I get up and *maybe* feel a tiny bit more headachy but no sleep impacts, which was my big worry. I'm just getting my hair back and at least so far no hair impacts. That was another concern. FWIW—a lot of women post about when in the day they take it—some prefer mornings, some prefer evenings. I've been taking it at midday (I do some intermittent fasting and generally don't eat breakfast) and that's been working well for me. I also take Biotin then (which I started before dx) and Vitamin D—it's easy for me to remember to take three pills at once. A calcium supplement was recommended but they make me nervous so I've been trying to increase the calcium in my diet.
0 -
Hi Wised - regarding starting hormone therapy early, I've gotten the impression it doesn't really matter how soon you start. My MO wrote the tamoxifen prescription at my surgical follow-up when she referred me to the radiologist, and the pharmacy notified me it was ready for pickup before I eveb got home from my appointment! But the PA, the nurse navigator, and at least one other person in the know told me that my MO is unusual in prescribing that soon, and most other oncologists just wait until everything else is done to avoid too many side effects at once. I asked why she does this, in case there was a reason, and they all sort of shrugged and said it's just what she does.
Pebbles - I've been slacking off on diet and exercise for the past few years due to some other heath and life distractions. Things aren't dreadful, but I could definitely make some improvements, and in a way, this is reassuring at the moment. There actually ARE things I can do to lower my risk. Of course there are super-fit vegans who get breast cancer, so I know it won't be any sort of guarantee, but I'll take any sense of control I can get at the moment.
Has anyone else asked their doctor about soy or flaxseed? I specifically asked, because I was confused by too much conflicting research, and was told that soy is fine in moderation but not to overdo and definitely don't make a point of eating more soy. I was also told that flaxseed has been shown to boost the effects of tamoxifen in certain circumstances, but the category into which I fall was not part of the study (or studies?)
0 -
Library girl, I also have osteoarthritis especially my right knee and left thumb. I spin my own yarn, knit, and weave. since I have been on anastrozole, I have noticed a slight worsening of those joint pains, but I continue to knit. I haven't tried spinning or weaving yet, but that's more because of the fatigue from radiation.I'm not letting this disease take everything from me. We need to continue doing those things that give us a good quality of life. If your treatment starts to impinge upon your quality of life let your oncologist know right away.
0 -
Spoonie, Dani, I'm so glad everyone is here!

MDRR, I really think physical activity is the key for most of us. My goal is to start my walking program and join a local gym when I start Christmas break. I really hope to reduce the side effects from Anastrazole. Thank you for the info on Fosteum. My MO wants me to start Prolia, but I'm a bit afraid of the side effects.
Ana, things have changed a bit in the sex department, but it's still good. Think quality over quantity.
Pebbles, I would love to take Tamoxifen, it's what my mom took for five years with few to no SE's. But tamoxifen is not compatible with Zoloft, so that's a no go for me.
Canada Liz, thank you for sharing your experience with Tamoxifen! I had no idea that could compromise your liver. That is really important to know especially if someone has taken chemotherapy prior to taking tamoxifen. So everyone, make sure your liver enzymes are check before you begin therapy.
it is just a boring, rainy, lazy Sunday here for me. It's morning, so I am having absolutely no leftover side effects from radiation. But I have a feeling that at about 2 o'clock I will get angry red and start to ache.
0 -
Just re: soy, I was also told not to worry about it as long as it’s not a major part of my diet.
0 -
Ingerp, Sorry I missed your previous post. Glad to hear about the soy. I love edamame, but have steered clear since my dx showed that my super power is converting androgens into estrogen. (I want a t-shirt)
0 -
Hi all,
RE: soy and other foods, I found this great site called https://foodforbreastcancer.com/amp/food-list.php that projects whether something is recommended or not to fight breast cancer based on the scientific studies that have been done. It's been super helpful for me and part of why I've cut red meat, dairy, processed foods and sugar (for now, not forever on the red meat and dairy). I'm eating morefruits and veggies, carrots and berries and garlic and turmeric especially good, says soy and flaxseed OK in moderation.
Purplecat - same here! Actually since being married (just 3.5 years ago) I think I gained 10 lbs a year. I don't mind thinking that there could be a link between the obesity and sugar (I used to go to work and put 5 packs of sugar in my coffee daily and if there were donuts in the office, I was first in line!) and lump I found in my breast because it means that I have the power to turn that around, and maybe I could keep it from coming back by getting super healthy and vigilant. Now I drink tea and not coffee, and I've gone through periods of getting super fit before so I know what to do. Positive - since the diagnosis back in August, I've lost 25 lbs! I've taken myself from an obese BMI to an overweight BMI so there's more to go. I told the oncologist I wanted to lose 20-25 more lbs and he actually looked at me and said that 10 more should be just fine, so I promised him I'd go for 10 and we could re-evaluate then. I'm only 5 ft and I got to the point where I don't LOOK overweight, I have a flat stomach now and look normal, but that dang BMI index says that the healthy range for me would be another 20-25 lbs to go. 😦
Wised - this quote from you rocks and I agree! “I'm not letting this disease take everything from me. We need to continue doing those things that give us a good quality of life.“ - I just love that strong power statement. So sorry tamoxifen is not an option, hopefully there's a different alternative for you. Letrozole?
Raysal - if it's up to you I recommend waiting til rads are done and letting your body adjust to one thing at a time. My radiologist actually insisted I not start tamoxifen with rads because he didn't want me to blame tamoxifen side effects on radiation treatment. I skated through radiation really well, no fatigue, tanned and not burnt skin, no nausea, did get a blister and some scratchy marks where I missed lotioning but it's very superficial, doesn't bother me.
Canadaliz - thank u for posting that story and warning and so sorry that happened to you. I had no idea there was potential impact on the liver too. Researching it now.
Ingerp - every other day sounds like a great way to ease into it and good to know that's been working for you. I'm also going to start tamoxifen at 10 mgs for a month and work my way up to 20 mgs which doc is good with
0 -
Hello, I started Anastrozole in Dec. 10. Had BMX, chemo and rads. All done before Thanksgiving. Now just AI and Lupron shots. Thinking about removing my ovaries, but didn’t make a decision yet. I am 46 and was pre-menopausal before chemo.
0 -
Ana001, InnaB2018, Mdrr, BeingPositive, and Thecargirl --> Welcome to the thread! <waves>
Good to see familiar faces here as well -- here's looking at you Alice, Ghostie, Appyfan, Purplecat, Librarygirl and Egregious! <waves some more>
Pebbles - LOL at the description of your sex life! NOT TMI at all IMO, but so glad to hear that you both are
still having fun, even if it's slightly less crazy than usual!
 And of course, thanks for the Domino dose for the day! Can't have enough of her, EVER!
And of course, thanks for the Domino dose for the day! Can't have enough of her, EVER! Raysal - FWIW, I was going to wait to start any type of hormone therapy until RADs was over. My MO rxed it
for me right at the beginning but I wanted to be sure I could tell what SEs were from what. They were fine with my waiting and I'm thankful I did because RADs was a tough ride for me. If I were you, I would simply ask your MO if it'd be ok to delay (if you want) for a week or two to see how RADs treats you. Couldn't hurt IMO. Wishing you the best of luck on your RADs journey!
CanadaLiz - Thank you thank you thank you for sharing your experience with Tamoxifen. I'm so sorry
about the troubles and permanent damage it brought into your world. Uggggh! It's reassuring news that your sons are a match for you but yet troubling since the transplant team won't allow transplant until after 5 years free of BC and your liver will possibly fail prior to that. You will be in my thoughts and so will your liver!
I can't even imagine having my liver fail on top of everything else I struggle with. Even though I had decided Tamoxifen was a no go for me prior to hearing your experience, it definitely reassured me that I made the best choice for myself. My liver already has issues and functions at about 75% when it was checked prior to LUMP in August. Yet, NO ONE mentioned to me in all the discussions about Tamox that there is a risk (2.9% may be "low" but it is a significant risk IMO) of liver damage with taking it. SMH. That should have been top of the list given my med history if you ask me.
So, yes please EVERYONE be sure to ask about having a baseline panel, including liver enzymes before starting hormone therapy.
0 -
Hey again everyone...
Because of CanadaLiz's experience on Tamoxifen regarding her liver (thank you again, DEEPLY, for sharing) I have been researching.
Sorry, not sorry.

Cross posting here for everyone's benefit.
Symptoms and Studies listed below.
I am utterly staggered by the studies that show the impact Tamoxifen has on the liver and the direct statements that EVERYONE should be clinically advised and monitored regarding their liver, as a baseline, and every 4 months thereafter. Yet, it seems to me, no one has really been told this or been tested for this?
Curious how many of you were informed of this risk (30-40% of developing Non-Alchoholic Fatty Liver Disease due to Tamoxifen) beforehand and also how many were tested/monitored for this danger/risk????
--------------
(cross posted)
Symptoms to be aware of:
https://www.breastcancer.org/treatment/side_effects/liver_probs
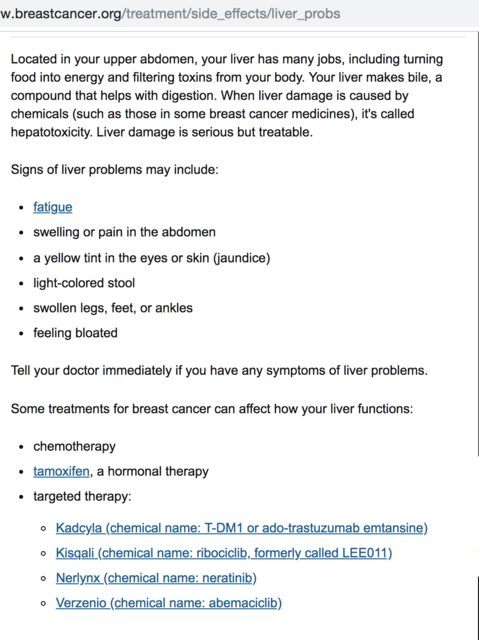
Here are a few studies for info:
A prospective, randomized study on hepatotoxicity of anastrozole compared with tamoxifen in women with breast cancer
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4462391/
"In addition, fatty liver disease, also known as non-alcoholic fatty liver disease (NAFLD) or non-alcoholic steatohepatitis (NASH), was observed in more than 30% of patients with breast cancer who received tamoxifen as adjuvant therapy.10,11 The first anastrozole-induced hepatotoxicity case was reported in 2006.12 A retrospective study demonstrated that fatty liver disease detected using ultrasound was more frequently seen with tamoxifen than with anastrozole (30.4% vs 6.25%).13 "Association between tamoxifen treatment and the development of different stages of nonalcoholic fatty liver disease
https://www.ncbi.nlm.nih.gov/pubmed/26071793
https://www.sciencedirect.com/science/article/pii/S092966461500176X
"Several studies showed that taking tamoxifen may incur a 30–40% risk of developing nonalcoholic fatty liver disease(NAFLD), according to different diagnosis instruments."ConclusionThe current study suggests that tamoxifen treatment is associated with the risk of fatty liver either by increasing the risk of newly developed fatty liver conditions or worsening previous fatty liver conditions, and even retarding fatty liver improvement."
"Our study suggests that tamoxifen is associated with the risk of NAFLD development, either by increasing the developed fatty liver or worsening the previous fatty liver condition and even retarding fatty liver improvement. The severity of fatty liver is associated with higher rates of abnormal LFT. During the follow-up period, regular abdominal ultrasound checkup, not just for detecting liver nodules, but also for identifying fatty liver change, is crucial. Further checking of liver function and other metabolic conditions once the fatty liver condition has progressed is essential."

Drug Record: Tamoxifen
https://livertox.nih.gov/Tamoxifen.htm
"Outcome and ManagementWhile fatty liver arises in at least one third of women treated with tamoxifen for up to 5 years, clinically significant steatohepatitis is less common. Nevertheless, monitoring of serum aminotransferase levels during tamoxifen therapy is appropriate. In women with persistent elevations in ALT levels, the relative benefits and risks of continuing tamoxifen therapy must be weighed. Factors to help in the decision, include noninvasive tests for hepatic fibrosis (platelet count), imaging of the liver and, in some instances, liver biopsy. Other approaches short of stopping tamoxifen therapy include nutritional advice and weight loss, abstinence from alcohol, and possibly medical therapies for nonalcoholic steatohepatitis (which are currently investigational and have not been shown to be specifically helpful in tamoxifen induced fatty liver). The possible development of serious hepatic fibrosis and portal hypertension can be assessed noninvasively by serial determinations of platelet count, but may require liver biopsy to document."
Tamoxifen induces hepatotoxicity and changes to hepatocyte morphology
https://www.spandidos-publications.com/10.3892/br.2015.536
"Clinically, patients who accept the endocrinotherapy are instructed to reexamine their liver function every 4 months due to its hepatotoxicity. Numerous research and clinical studies have illustrated clearly that TAM causes the inhibition of mitochondrial β-oxidation and subsequently leads to macrovacuolar steatosis (21,22). The early symptoms were characterized by the presence of a single, large lipid vacuole within the cytoplasm of the hepatocytes (23)."
"In conclusion, the present data showed that a relatively low concentration of TAM (6 mg/kg/day) for a short time treatment (2 weeks) would cause hepatotoxicity and change morphology at the microscopic and ultrastructural levels. Although the liver function may compensate or reverse the injuries gradually, the damage that occurred in the short-term TAM therapy has been shown. Thus, there is a necessity to obtain measures for monitoring liver function and protection at the early stage of the TAM endocrinotherapy, prior to apparent and undesirable clinical symptoms occurring. Furthermore, as DNA damage also occurs at this early period without clear clinical symptoms, which in the long-run increases the risk of hepatocarcinoma, exploring alternatives for TAM in long-term clinical endocrinotherapy is required."
Liver Injury Induced by Anticancer Chemotherapy and Radiation Therapy
https://www.hindawi.com/journals/ijh/2013/815105/

Death due to liver failure during endocrine therapy for premenopausal breast cancerhttps://www.tandfonline.com/doi/full/10.3109/0284186X.2010.484813"In the tamoxifen product information, liver-related side effects are listed and it is recommended to perform periodic liver function tests, although in clinical practice blood tests are no longer performed routinely during follow-up for women with early breast cancer."
"Young women, in particular between ages 26 to 35, seem to be—for yet unknown reasons—more frequently affected by acute liver failure, and the use of antidepressants (metabolized primarily via liver enzymes CYP 3A4, 2D6, 2C19), other potentially hepatotoxic drugs (e.g. acetaminophen-type analgesics and NSAIDs), and alcohol are more frequent in younger breast cancer patients than generally presumed and reported. We therefore advise physicians to pay special attention to patients treated with endocrine therapy for breast cancer who have concurrent depression and who potentially or actively consume hepatotoxic drugs and alcohol. Such patients should have their liver function monitored and liver imaging should be performed if indicated."
The Association of Nonalcoholic Steatohepatitis and Tamoxifen in Patients With Breast Cancer
https://onlinelibrary.wiley.com/doi/pdf/10.1002/cncr.24374
A prospective, randomized study on hepatotoxicity of anastrozole compared with tamoxifen in women with breast cancer
https://pdfs.semanticscholar.org/3aa1/d236d38c20f3a9377dea6f9d5ad8235221c6.pdf
G.L.O.W.N. - Tamoxifen
https://www.glowm.com/resources/glowm/cd/pages/drugs/t002.html
"Effects on lab test results
• May increase BUN, calcium, and liver enzyme levels.
• May decrease WBC and platelet counts.Special considerations
• Tamoxifen acts as an antiestrogen. Best results occur in patients with positive estrogen receptors.
• Adverse reactions are usually minor and well tolerated. They usually can be controlled by dose reduction. ALERT Serious, life-threatening, or fatal events associated with tamoxifen in the risk reduction setting include endometrial cancer, uterine sarcoma, stroke, and pulmonary embolism.
ALERT Serious, life-threatening, or fatal events associated with tamoxifen in the risk reduction setting include endometrial cancer, uterine sarcoma, stroke, and pulmonary embolism.  ALERT Discuss the potential benefits versus the potential risks with women considering treatment to reduce their risk of developing breast cancer. Benefits of therapy outweigh risks in women diagnosed with breast cancer.
ALERT Discuss the potential benefits versus the potential risks with women considering treatment to reduce their risk of developing breast cancer. Benefits of therapy outweigh risks in women diagnosed with breast cancer.
• Clotting factor abnormalities may occur with prolonged tamoxifen therapy at usual doses.
• Variations on karyopyknotic index in vaginal smears and various degrees of estrogen effect on Papanicolaou smears have been seen in some postmenopausal patients. May increase serum thyroxine concentrations and may be explained by increases in thyroxine-binding globulin.
• Initial adverse reactions (increased bone pain) may be a sign of good tumor response shortly after starting tamoxifen therapy.
• Monitor WBC count, platelet count, and periodic liver function tests results.
• Monitor serum calcium levels; hypercalcemia may occur early in therapy in patients with bone metastases."0